7 June 2020
Geneva Scientist Invents Wearable Life Support to Change Critical Care
Andriy Batchinsky, MD is pioneering advancements in extracorporeal life support, focusing on combat and civilian trauma and novel critical care interventions, to save lives both on and off the battlefield.
“Do with what you have – that’s where battlefield medicine is going today. Medical preparedness cannot assume unlimited supplies are available, which is extremely relevant now with COVID-19,” said Andriy Batchinsky, MD. “The biggest challenge I have is explaining to people with a peacetime mentality how to prepare for a wartime medical situation or a mass casualty situation like COVID-19 and do so with the realistic expectations.”
Dr. Batchinsky is a trauma surgeon by education and translational scientist at heart. A Geneva researcher since 2014, he is also the founder and director of the Autonomous Reanimation and Evacuation (AREVA) Research Program, where various Geneva research projects are carried out in San Antonio, Texas. In addition, he is the Extracorporeal Life Support (ECLS) Capability Area Manager at the U.S. Army Institute of Surgical Research (USAISR) at Fort Sam Houston where he has conducted research since January 2001.
Beginning his career as a surgeon in the Ukraine, he practiced medicine in underdeveloped conditions with few resources, which he credits with sparking his passion for battlefield medicine. He attributes his drive to create better research for combat environments and his 19 years in combat casualty care in various roles to the late Professor of Surgery, Basil Pruitt Jr., MD, former commander and director of the USAISR, who first introduced Batchinsky to the Institute in 1998. Together with the current director Lee Cancio MD, they have been a big influence in Dr. Batchinsky’s career at USAISR.
Dr. Batchinsky has a special interest in minimally invasive ECLS for treatment of lung and multiorgan failure in combat and civilian trauma, as well as resuscitation of patients with massive severe combined injuries and exsanguination: simply put he wants to save those that others deem to be unsavable.

ECLS was not a core Army objective until the last year. Today, the Department of Defense recognizes that ECLS can save lives early instead of last resort measures. “We now have more advanced forms of ECLS and an existence of a program within the DoD which paves the way for earlier implementation of lifesaving technologies in combat and civilian care alike,” added Batchinsky.
Mechanical ventilation remains the current standard of therapy for failing lungs during the COVID -19 pandemic and a commonly used support modality for the critically ill with other problems. Dr. Batchinsky has set out to introduce modern lung support and renal replacement technologies in wearable format and without the need for mechanical ventilators which, in his opinion, will be ousted from hospitals in a few years. Batchinsky’s invention, the Combat Resuscitation Organ Support System (CROSS) is a wearable vest for which he and his team members filed an invention disclosure last year, well before COVID-19 made its way around the globe. He believes the CROSS device could revolutionize intensive care units (ICU) for patients suffering from coronavirus or any other severe respiratory illness requiring intubation and mechanical ventilation saying, “Those COVID patients who end up in ICUs on ventilators had an 88% death rate in older, obese, hypertensive patients in New York. This current standard of care is the best we got but completely contradicts to natural breathing patterns of humans and should be replaced with direct oxygenation and Co2 removal e.g. breathing carried out in the blood by ECLS.”
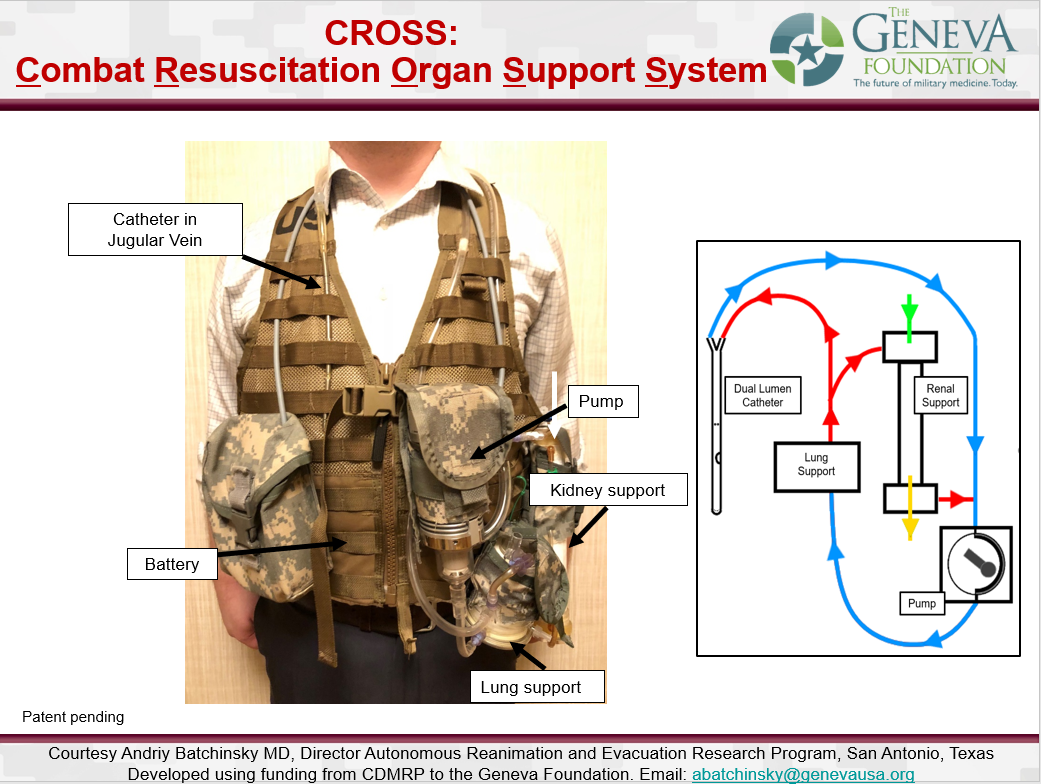
The CROSS is a lung and renal support device connecting to patients by a catheter. It replaces lung function and renal function. The CROSS will permit patients to receive ambulatory care at home or at the point-of-injury, reducing the need for ICU beds, and allowing patients to be free of ventilators while conscious and mobile.
“It is the potential answer to multiple Army objectives,“ said Dr. Batchinsky. This device can make ECLS therapy for lung injuries available during critical care ground and air evacuation, and close to the point of the time of injury, easily fitting into ground evacuation vehicles and aircraft. “It’s a game-changer which will permit injured to walk, talk and actively recuperate and for many to remain operationally functional on the battlefield.”
This is not the first time Dr. Batchinsky has pioneered the applications of techniques to address the Department of Defense’s trauma models.
At the AREVA program located in a San Antonio Brooks City Base facility, Batchinsky leads a multi-disciplinary research team of 15 people engaged in translational research focusing on combat-relevant trauma and novel critical care interventions for combat casualties during care at ground level and high altitudes.
“This unique research platform doesn’t exist anywhere in the world,” he said. “Our team is able to replicate difficult situations from critical care and implications of altitudes and we have ICU animal expertise to mimic around-the-clock human-like conditions. I feel as though my team, most of whom have no formal medical education, could perform in any ICU in any critical care condition and be successful.”
Dr. Batchinsky operates his team and lab at a more programmatic level instead of a project-by-project basis. He hires and retains people to support the mission, gladly shouldering the responsibility of preparing his team members for careers in medicine or elsewhere. He feels personally responsible for making sure his team members learn life-long skills and those that stay in his lab never have to worry about employment again.
“Never do I feel as relevant as I do right now,” said Dr. Batchinsky. “Geneva drives medicine and can be the main conduit of medical innovation during this time of uncertainty. My AREVA team consists of dedicated to research young men and women and one day soon we will change medical care in the world.”
Dr. Batchinsky’s views do not represent those of the U.S. Army, Department of Defense, or U.S. Government.
"We now have more advanced forms of ECLS and an existence of a program within the DoD which paves the way for earlier implementation of lifesaving technologies in combat and civilian care alike."
Andriy Batchinsky, MD, Research Scientist
HIGHLIGHTS
- Dr. Batchinsky has a special interest in minimally invasive ECLS for treatment of lung and multiorgan failure in combat and civilian trauma, as well as resuscitation of patients with massive severe combined injuries and exsanguination.
- He has set out to introduce modern lung support and renal replacement technologies in wearable format which could revolutionize intensive care units (ICU) for patients suffering from coronavirus or any other severe respiratory illness requiring intubation and mechanical ventilation. Batchinsky’s invention is a wearable vest called the Combat Resuscitation Organ Support System (CROSS).
- At the AREVA laboratory, Batchinsky leads a multi-disciplinary research team of 15 people engaged in translational research focusing on combat-relevant trauma and novel critical care interventions for combat casualties during care at ground level and high altitudes.


